Stopping Sepsis: Understanding the Signs and Symptoms
Sepsis is like an ember that sparks from a small campfire, suddenly threatening the whole forest. If not treated early, it can progress into septic shock. The…

Update your location to show providers, locations, and services closest to you.
Chills refers to feeling cold after being in a cold environment. The word can also refer to an episode of shivering along with paleness and feeling cold.
Rigors; Shivering
Chills (shivering) may occur at the start of an infection. They are most often associated with a fever. Chills are caused by rapid muscle contraction and relaxation. They are the body's way of producing heat when it feels cold. Chills often predict the coming of a fever or an increase in the body's core temperature.
Chills are an important symptom with certain diseases such as malaria.
Chills are common in young children. Children tend to develop higher fevers than adults. Even minor illness can produce high fevers in young children.
Infants tend not to develop obvious chills. However, call your health care provider about any fever in an infant 6 months or younger. Also call for fevers in infants 6 months to 1 year unless you are sure of the cause.
"Goose bumps" are not the same as chills. Goose bumps occur due to cold air. They can also be caused by strong emotions such as shock or fear. With goose bumps, the hair on the body stick up from the skin to form a layer of insulation. When you have chills, you may or may not have goose bumps.
Causes may include:
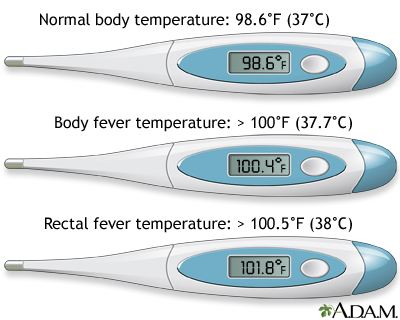
Fever (which can accompany chills) is the body's natural response to a variety of conditions, such as infections. If the fever is mild, 102°F (38.8°C) or less, with no side effects, you do not need to see a provider for treatment. You can treat the problem at home by drinking lots of fluids and getting plenty of rest.
Evaporation cools the skin and reduces body temperature. Sponging with lukewarm water, about 70°F (21.1°C), may help reduce a fever. Cold water may increase the fever as it can trigger chills.
Medicines such as acetaminophen are helpful in fighting a fever and chills.
DO NOT bundle up in blankets if you have a high temperature. DO NOT use fans or air conditioners either. These measures will only make the chills worse and may even cause the fever to rise.
HOME CARE FOR A CHILD
If the child's temperature is causing the child to be uncomfortable, give pain-relieving tablets or liquid. Non-aspirin pain-relievers such as acetaminophen are recommended. Ibuprofen may also be used. Follow the dosage guidelines on the package label.
Note: DO NOT give aspirin to treat fever in a child younger than 19 years old because of the risk for Reye syndrome.
Other things to help the child feel more comfortable include:
Call the provider if:
The provider will take your medical history and perform a physical exam.
You may be asked questions such as:
The physical exam will include the skin, eyes, ears, nose, throat, neck, chest, and abdomen. Body temperature will likely be checked.
Tests that may be ordered include:
Treatment depends on how long the chills and accompanying symptoms (especially fever) have lasted.
American Academy of Pediatrics website. Fever. www.healthychildren.org/English/health-issues/conditions/fever/Pages/default.aspx. Accessed April 12, 2021.
Hall JE, Hall ME. Body temperature regulation and fever. In: Hall JE, Hall ME, eds. Guyton and Hall Textbook of Medical Physiology. 14th ed. Philadelphia, PA: Elsevier; 2021:chap 74.
Leggett JE. Approach to fever or suspected infection in the normal host. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 264.
Nield LS, Kamat D. Fever. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 201.
Sepsis is like an ember that sparks from a small campfire, suddenly threatening the whole forest. If not treated early, it can progress into septic shock. The…

July 10, 2023
A new project from the University of Florida College of Medicine is aimed at screening patients ahead of scheduled surgeries to improve their recovery time and…
Department of Anesthesiology, Department of Surgery, +2 more
Ever zoned out in the car on a Saturday morning and started to drive to work when you meant to go to the grocery store for milk? It happens. According to memory experts, the part of your brain...
Having alcohol easily available may be handy for young adults, but it certainly can mean a lot of heartache for youngsters. A new research study led by researchers at Ohio State University examined...
Go ahead, pile on the chili peppers. It just might help your heart stay healthy. Findings by researchers in Italy suggest that regular consumption of chili peppers may reduce the long-term risk of...