Understanding your risk for pancreatic cancer
In 2021 alone, an estimated 60,430 Americans will be diagnosed with pancreatic cancer in the U.S., and nearly all will die from the disease. A pancreatic…

Update your location to show providers, locations, and services closest to you.
Pancreatitis is swelling of the pancreas. Chronic pancreatitis is present when this problem does not heal or recurs and does not improve, gets worse over time, and leads to permanent damage.
Chronic pancreatitis - chronic; Pancreatitis - chronic - discharge; Pancreatic insufficiency - chronic; Acute pancreatitis - chronic
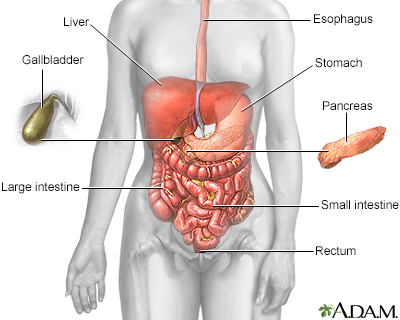
The pancreas is an organ located behind the stomach. It produces chemicals (called enzymes) needed to digest food. It also produces the hormones insulin and glucagon.
When scarring of the pancreas occurs, the organ is no longer able to make the right amount of these enzymes. As a result, your body may be unable to digest fat and key elements of food.
Damage to the parts of the pancreas that make insulin may lead to diabetes mellitus.
The condition is most often caused by alcohol abuse over many years. Repeated episodes of acute pancreatitis can lead to chronic pancreatitis. Genetics may be a factor in some cases. Sometimes, the cause is not known or caused by gall stones.
Other conditions that have been linked to chronic pancreatitis:
Chronic pancreatitis is more common in men than in women. This often occurs in people ages 30 to 40.
Symptoms include:
DIGESTIVE PROBLEMS
Tests to diagnose pancreatitis include:
Tests that may show the cause of pancreatitis include:
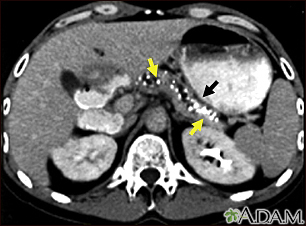
Imaging tests that can show swelling, scarring, calcifications or other changes of the pancreas may be seen on:
ERCP is a procedure that looks at your bile and pancreatic ducts. It is done through an endoscope.
People with severe pain or who are losing weight may need to stay in the hospital for:
The right diet is important for people with chronic pancreatitis to keep a healthy weight and get the correct nutrients. A nutritionist can help you create a diet that includes:
The health care provider may prescribe pancreatic enzymes. You must take these medicines with every meal, and even with snacks. The enzymes will help you digest food better, gain weight and reduce diarrhea.
Avoid smoking and drinking alcoholic beverages, even if your pancreatitis is mild.
Other treatments may involve:
Surgery may be performed if a blockage is found. In severe cases, a part of or the entire pancreas may be removed.
This is a serious disease that may lead to disability and death. You can reduce the risk by avoiding alcohol.
Complications may include:
Contact your provider if:
Finding the cause of acute pancreatitis and treating it quickly may help prevent chronic pancreatitis. Limit the amount of alcohol you drink to reduce your risk of developing this condition.
Forsmark CE. Chronic pancreatitis. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/Management. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 59.
Forsmark CE. Pancreatitis. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 135.
Lancaster WP, Adams DB. Management of chronic pancreatitis. In: Cameron AM, Cameron JL, eds. Current Surgical Therapy. 13th ed. Philadelphia, PA: Elsevier; 2020:541-545.

In 2021 alone, an estimated 60,430 Americans will be diagnosed with pancreatic cancer in the U.S., and nearly all will die from the disease. A pancreatic…

Dear colleagues, In the Division of Gastroenterology, Hepatology and Nutrition at University of Florida Health, we run a comprehensive program that covers the…
