Malignant hypertension
Definition
Malignant hypertension is very high blood pressure that comes on suddenly and quickly.
Alternative Names
Accelerated hypertension; Arteriolar nephrosclerosis; Nephrosclerosis - arteriolar; Hypertension - malignant; High blood pressure - malignant
Causes
The disorder affects a small number of people with high blood pressure, including children and adults. It is more common in younger adults, especially African American men.
It also occurs in people with:
- Collagen vascular disorders (such as systemic lupus erythematosus, systemic sclerosis, and periarteritis nodosa)
- Kidney problems
- Pregnancy-induced high blood pressure (toxemia)
You are at high risk for malignant hypertension if you smoke and if you have had:
- Kidney failure
- Renal hypertension caused by renal artery stenosis
Symptoms
Symptoms of malignant hypertension include:
- Blurred vision
- Change in mental status, such as anxiety, confusion, decreased alertness, decreased ability to concentrate, fatigue, restlessness, sleepiness, or stupor
- Chest pain (feeling of crushing or pressure)
- Cough
- Headache
- Nausea or vomiting
- Numbness of the arms, legs, face, or other areas
- Reduced urine output
- Seizure
- Shortness of breath
- Weakness of the arms, legs, face, or other areas
Exams and Tests
Malignant hypertension is a medical emergency.
A physical exam commonly shows:
- Extremely high blood pressure
- Swelling in the lower legs and feet
- Abnormal heart sounds and fluid in the lungs
- Changes in thinking, sensation, and reflexes
An eye exam will reveal changes that indicate high blood pressure, including:
- Bleeding of the retina (back part of the eye)
- Narrowing of the blood vessels in the retina
- Swelling of the optic nerve
- Other problems with the retina
Tests to determine damage to the kidneys may include:
- Arterial blood gas analysis
- BUN (blood urea nitrogen)
- Creatinine
- Urinalysis
- Kidney ultrasound
A chest x-ray may show congestion in the lungs and an enlarged heart.
This disease may also affect the results of these tests:
- Level of aldosterone (a hormone from the adrenal gland)
- Cardiac enzymes (markers of heart damage)
- CT scan of the brain
- Electrocardiogram (ECG)
- Renin level
- Urinary sediment
Treatment
You will need to stay in the hospital until your severe high blood pressure is under control. You will receive medicines through a vein (IV) to reduce your blood pressure.
If there is fluid in your lungs, you will be given medicines called diuretics, which help the body remove fluid. Your doctor may give you medicines to protect your heart if you have signs of heart damage.
After your severe high blood pressure is under control, blood pressure medicines taken by mouth can control blood pressure. Your medicine may need to be changed sometimes. High blood pressure can be difficult to control.
Outlook (Prognosis)
Many body systems are at serious risk from the extreme rise in blood pressure. Organs including the brain, eyes, blood vessels, heart, and kidneys may be damaged.
The blood vessels of the kidney are very likely to be damaged by high blood pressure. Kidney failure may develop, which may be permanent. If this happens, you may need dialysis (machine that removes waste products from blood).
If treated right away, malignant hypertension can often be controlled without causing permanent problems. If it is not treated right away, it can be fatal.
Possible Complications
These complications may occur:
- Brain damage (stroke, seizures)
- Heart damage, including: heart attack, angina (chest pain due to narrowed blood vessels or weakened heart muscle), heart rhythm disturbances
- Kidney failure
- Permanent blindness
- Fluid in the lungs
When to Contact a Medical Professional
Go to the emergency room or call the local emergency number (such as 911) if you have symptoms of malignant hypertension. This is an emergency condition that can be life threatening.
Contact your health care provider if you know you have poorly controlled high blood pressure.
Prevention
If you have high blood pressure, carefully monitor your blood pressure and take your medicines properly to help reduce your risk. Eat a healthy diet that is low in salt and fat.
Gallery
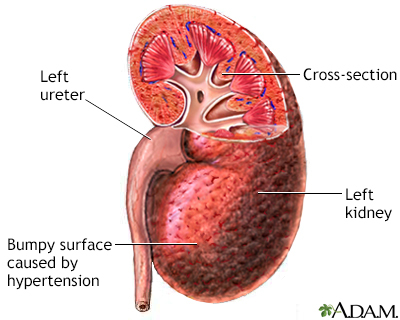
References
Elliott WJ, Peixoto AJ, Bakris GL. Primary and secondary hypertension. In: Yu ASL, Chertow GM, Luyckx VA, Marsden PA, Skorecki K, Taal MW, eds. Brenner and Rector's The Kidney. 11th ed. Philadelphia, PA: Elsevier; 2020:chap 46.
Greco BA, Umanath K. Renovascular hypertension and ischemic nephropathy. In: Feehally J, Floege J, Tonelli M, Johnson RJ, eds. Comprehensive Clinical Nephrology. 6th ed. Philadelphia, PA: Elsevier; 2019:chap 41.
Levy PD, Brody A. Hypertension. In: Walls RM, Hockberger RS, Gausche-Hill M, eds. Rosen's Emergency Medicine: Concepts and Clinical Practice. 9th ed. Philadelphia, PA: Elsevier; 2018:chap 74.
