Common Questions About Multiple Sclerosis
More than 900,000 adults in the United States are living with multiple sclerosis, according to the National Multiple Sclerosis Society. The multiple sclerosis…
Update your location to show providers, locations, and services closest to you.
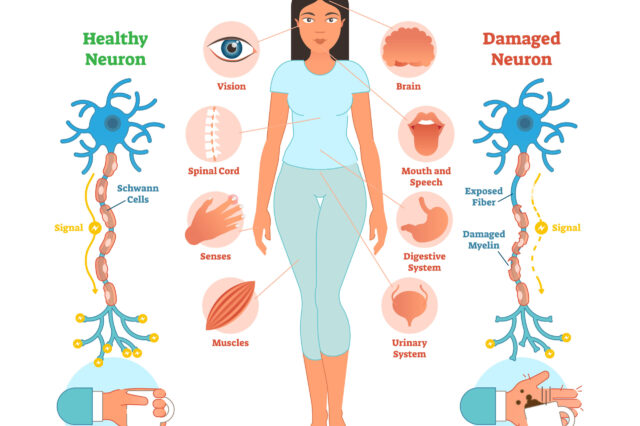
Neuralgia is a sharp, shocking pain that follows the path of a nerve and is due to irritation or damage to the nerve.
Common neuralgias include:
Nerve pain; Painful neuropathy; Neuropathic pain
Causes of neuralgia include:
In many cases, the cause is unknown.
Postherpetic neuralgia and trigeminal neuralgia are the two most common forms of neuralgia. A related but less common neuralgia affects the glossopharyngeal nerve, which provides feeling to the throat.
Neuralgia is more common in older people, but it may occur at any age.
Symptoms may include any of the following:
The health care provider will perform a physical exam, and ask about your symptoms.
The exam may show:
You may also need to see a dentist if the pain is in your face or jaw. A dental exam can rule out dental disorders that may cause facial pain (such as a tooth abscess).
Other symptoms (such as redness or swelling) may help rule out conditions such as infections, bone fractures, or rheumatoid arthritis.
There are no specific tests for neuralgia. But, the following tests may be done to find the cause of the pain:
Treatment depends on the cause, location, and severity of the pain.
Medicines to control pain may include:
Other treatments may include:
Procedures may not improve symptoms and can cause loss of feeling or abnormal sensations.
When other treatments fail, doctors may try nerve or spinal cord stimulation. In rare cases, a procedure called motor cortex stimulation (MCS) is tried. An electrode is placed over part of nerve, spinal cord, or brain and is hooked to a pulse generator under the skin. This changes how your nerves signal and it may reduce pain.
Most neuralgias are not life threatening and are not signs of other life-threatening disorders. For severe pain that does not improve, see a pain specialist so that you can explore all treatment options.
Most neuralgias respond to treatment. Attacks of pain usually come and go. But, attacks may become more frequent in some people as they get older.
Sometimes, the condition may improve on its own or disappear with time, even when the cause is not found.
Complications may include:
Contact your provider if:
Strict control of blood sugar may prevent nerve damage in people with diabetes. In the case of shingles, antiviral drugs and the herpes zoster virus vaccine may prevent neuralgia.
Katirji B. Disorders of peripheral nerves. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff’s Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 106.
Scadding JW, Koltzenburg M. Painful peripheral neuropathies. In: McMahon SB, Koltzenburg M, Tracey I, Turk DC, eds. Wall and Melzack's Textbook of Pain. 6th ed. Philadelphia, PA: Elsevier Saunders; 2013:chap 65.
Smith G, Shy ME. Peripheral neuropathies. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 392.






More than 900,000 adults in the United States are living with multiple sclerosis, according to the National Multiple Sclerosis Society. The multiple sclerosis…

UF Health Pain Medicine has recently begun offering the SPRINT® peripheral nerve stimulation, or PNS, as a drug-free, minimally invasive way to block chronic…
