Unvaccinated, expectant mother nearly dies of COVID-19, becomes vaccine champion

Friends and family gathered at Amy Westman’s July 24 baby shower. Gifts and balloons and bursts of blue brightened the room. Blue cupcakes. Blue bows and wrapping paper. Blue as in boy. Her lovely Nicholas.
Amy didn’t give much thought to the coronavirus at the shower. Nicholas was six weeks from his due date. This was a happy time. All these months into the pandemic and she hadn’t gotten sick. Besides, the coronavirus seemed at low ebb.
“COVID had died down and everybody was starting to unmask,” said Amy’s sister, Tracey Shrine.
Amy, unvaccinated and unmasked, had undergone difficult fertility treatments to become a mother at age 45. Hers was a challenging pregnancy, and obstetricians at University of Florida Health monitored her closely. Amy wasn’t convinced about the safety of the COVID-19 vaccines. She didn’t want to take any chances.
“I just didn’t want to do anything to risk my baby,” the Dunnellon resident said.
The pleas of her vaccinated parents and sister, however, were beginning to sway her. Amy just might get that shot.
What followed that baby shower was an ordeal that shattered Amy’s sense that she lived a life apart the pandemic, untouched and unthreatened by a storm that had swept the country. The coming weeks would convince her that vaccines didn’t threaten a pregnancy. For a vaccinated mother, they might actually save it.
The Centers for Disease Control and Prevention, which recommends pregnant women get vaccinated, says 97% of hospitalized mothers-to-be infected with the coronavirus are unvaccinated.
Nicholas was Amy’s “miracle baby,” and she hoped angels watched over him. Perhaps at that baby shower, perhaps elsewhere, something besides angels floated invisibly in the air.
A few days later, Amy felt a tickle in the back of her throat.
* * *
Amy wasn’t alone in her reluctance.
Tony Wen, M.D., a professor in the UF College of Medicine’s department of obstetrics and gynecology, said he often finds himself trying to reassure wary expectant mothers that a COVID-19 vaccine is a potential lifesaver for mother and child.
Wen, chief of UF Health’s OB-GYN’s division of maternal-fetal medicine, said research has shown pregnancy itself can be a risk factor for developing severe COVID-19.
“For the mom, the chances of getting COVID pneumonia and requiring intubation and a ventilator is actually higher,” Wen said. “In this time of the delta variant, we see it quite often that an unvaccinated mother will deteriorate much faster.”
Many women worry the vaccine contains live virus that can be passed across the placenta, infecting the unborn baby. But this isn’t so, he said. No live virus is used in any COVID-19 vaccine.
And a complication of COVID-19 pneumonia, Wen noted, is the preterm delivery of low-weight babies.
Almost everyone hospitalized with COVID-19, and who die from it, are unvaccinated, or if vaccinated, immunocompromised.
“At this point it isn’t a maybe,” said Ali Ataya, M.D., a UF Health pulmonary critical care specialist and associate professor in the UF College of Medicine’s division of pulmonary, critical care and sleep medicine.
“We know from all the evidence, from everything that we see on a daily basis — vaccination is safe and saves patients from developing severe COVID infection. Almost all of our medical ICU patients on ventilators are unvaccinated.”
* * *
That tickle in Amy’s throat quickly blossomed into a sore throat, then a nagging cough.
Even so, she doubted she was infected by the coronavirus. Impossible, she thought.
“I worked from home,” said Amy, a sales coordinator for a human resources outsourcing company. “I’m a major homebody. I rarely go out and about traveling.”
Her condition, however, worsened. The wheezing in her chest worried her. The racking coughs became painful. She felt utterly exhausted doing normally easy household chores like the laundry. Breathing was becoming an ordeal.
Amy called UF Health and was urged to get a COVID-19 test.
She expected a negative result. Amy said she was a healthy person. “I had no comorbidity other than being pregnant and overweight.”
She stared at the test results on her computer screen in disbelief the next morning. That cough and exhaustion weren’t a summer cold.
Amy had COVID-19.
She posted on Facebook, “If you want to forget altogether that you are 35 weeks pregnant, just get COVID … literally I have never been so miserable in my entire life!!!!”
Her husband, Tim, also unvaccinated, developed a mild case of COVID-19. Amy’s vaccinated mother got a minor breakthrough case.
Worse than her symptoms, Amy wasn’t feeling her baby’s normally vigorous kicks and bumps. That scared her to death.
She went back to UF Health for an ultrasound. Nicholas was fine.
By Aug. 3, Amy had endured enough. She couldn’t sleep. The coughing and the panicked feeling of not being able to breathe overwhelmed her. It was clear she wasn’t going to get better on her own.
She told her husband, “We’ve got to call 911.”
* * *
A nurse from UF Health Shands’ labor and delivery unit sat with Amy at the hospital, trying to calm her so she could breathe more easily.
Doctors gave Amy oxygen. But nothing seemed to be helping, which scared her most of all. As different doctors and nurses examined her, Amy saw the same looks of deep concern etched in their faces. She understood what those eyes communicated.
“I knew I was in big trouble,” she said.
A doctor told Amy she needed an emergency Cesarean delivery. She and her baby were in danger. And she would need to go on a ventilator. Amy’s blood-oxygenation stood in the low 80% range, far too low to support her baby’s life, much less her own.
Ataya didn’t think Amy would pull through. Few people this ill did.
“She was in severe respiratory failure from COVID pneumonia,” Ataya said. “Her body was in shock. The lungs weren’t working. She even developed heart failure from the infection. We worried that neither she nor the baby would make it.”
Amy called her mother, Joanne Kriesel. It was early morning, the phone’s ringing awakening her.
“Mom,” Amy said, struggling to talk. “I’m at Shands. I came by ambulance. There’s some people here who want to talk to you.”
Joanne was flabbergasted. She knew Amy had COVID-19. But she was shocked at how quickly her condition had deteriorated. In that brief call, she heard the voice of a dying woman.
* * *
Wen and Michelle Larzelere, M.D., an assistant professor in the UF College of Medicine’s department of obstetrics and gynecology, delivered Nicholas with help from a resident.
The baby’s body, like Amy’s, was starved for oxygen. But he was alive.
Amy’s early days in the intensive care unit were filled with up and downs. Doctors used virtually their entire COVID-19 toolkit to try to save her.
Ataya said doctors needed to attempt different ways to improve Amy’s oxygenation and support her lungs. In addition to the mechanical ventilator, the medical team rolled Amy on her belly in a prone position for most of the day.
“This has been proven to help with a patient’s oxygen levels,” he said.
Amy also received steroids, antiviral and anti-inflammatory drugs to reduce the viral load in her body. Nurses continually suctioned secretions from her aggrieved lungs.
But with her doctors as with family, it was a waiting game. Every patient responds differently to COVID-19 and its treatments, Ataya said. Whether Amy would emerge from this assault on her lungs and body was maddeningly unpredictable.
“Once the patient is on a ventilator,” Ataya said, “it’s just about giving them time.”
Amy’s sister, Tracey, posted updates on Facebook, asking for prayers.
“For anyone who knows my sister personally, you know that she is a fierce and determined person ... even though she is sedated, I hope that her fighting spirit continues to prevail and will help her overcome the odds of this terrible situation!”
* * *
Nicholas, meantime, was in the neonatal intensive care unit.
At first, he was in isolation, the medical team fearful that, like his mother, he might be infected with the coronavirus. But tests eventually came back negative, and family could visit.
At birth the baby weighed 6 pounds, 15 ounces, a healthy weight for a child born a month early.
Nicholas was put on oxygen support. He was monitored for seizures, a common side effect of his low-oxygen entry into the world. But the boy, his family said, recovered quickly. In nine days, he would be discharged.
Tracey and her husband agreed to take him to their Tallahassee home. Nicholas’ father was a long-haul trucker on the road all week, and the family desperately needed his income.
For Amy, small improvements were seized upon by her family.
“Her nurses report that she is doing some breathing on her own even though she’s still on the ventilator — baby steps!” her sister posted Aug. 6 on Facebook. “Amy also responded to a verbal cue to squeeze the nurse’s hand, another great sign!”
Visitors weren’t allowed for COVID-19 patients. Nurses would hold a smartphone near Amy, sedated and unable to communicate, so family members could offer reassuring words.
“You’ll get through this,” Amy’s mother, Joanne, told her. “We all love you.”
Ups and downs followed. Amy developed bacterial pneumonia and a fever, undergoing a regimen of antibiotics. Doctors would try to wean her off the ventilator, only to be thwarted by her inflamed lungs.
The ventilator’s settings would be adjusted and then readjusted to provide more or less oxygen as Amy’s condition improved and worsened and then improved again. It was a fraught tug of war between life and death.
And in tiny increments, Amy started to get better.
The fever retreated. The ventilator wasn’t having to push out as much oxygen. Her level of sedation was decreased.
On the night of Aug. 16, a nurse asked Amy, still on the ventilator, to open her eyes.
It was a moment that answered a family’s prayers.
Amy’s eyes opened to her vastly changed life.
* * * Amy finally left the ICU on Aug. 24 after nearly three weeks. She would spend another three weeks in the hospital. Then she was discharged to the UF Health Rehab Hospital, where she would have to strengthen muscles weakened by disease and inactivity.
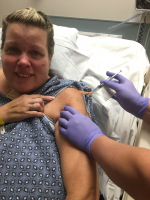
As she was taken by stretcher for the short trip, a nurse asked Amy if she wanted that COVID-19 vaccination. The shot could boost her antibody levels to offer greater protection than COVID-19 infection gave her by itself.
This time, there was no hesitation, no doubts about a vaccine’s safety. Amy got her shot. Painless. She experienced no side effects.
In the hospital, and then her room at the rehab hospital, large photos of Nicholas were taped to walls, the baby she had still not hugged or kissed or even touched.
Amy’s rehab was difficult. Her body needed to relearn how to move. She needed to build strength to care for the baby that awaited her.
Someone had written on a white board in the room Amy’s rehabilitation goal: “To feel strong and confident and be able to take care of my baby.”
On Oct. 1, after 58 days in the hospital and rehab, after nearly two months without touching or seeing her baby, after so much time forever lost to COVID-19, Amy’s most fervent wish was answered.
“Today is my rebirth, my second chance at life,” she said.
Amy was going home to see her Nicholas.
Amy’s sister handed over Nicholas outside Amy’s Dunnellon home after the drive from the hospital. The mother could hardly believe the boy was in her arms. She fought back tears.
“You’ve been with aunt Tracey for two months,” she said softly. “Now you’re with your mommy.”
A mother made her first bottle. She rocked her baby to sleep for the first time. She changed her first diaper as a mom. So many firsts to replace all those that the coronavirus erased.
She looked into her baby’s eyes.
“Do you know how much mommy loves you?”
* * *
Doctors say Amy’s caregivers were part of a huge multidisciplinary team. It included doctors, nurses and other staff in pulmonary and critical care medicine, emergency medicine, OB-GYN, the medical ICU, neonatal care, physical and occupational therapy, and respiratory therapy.
“If Amy had been vaccinated and then gotten COVID like she did, she probably would have felt like she had a really bad cold and probably nothing worse,” Ataya said. “The entire team is incredibly happy she and her baby Nicholas made it.”
Even with all her progress, Ataya said Amy still has a long road ahead for a full recovery.
Amy is thankful, and angry — at herself.
She said so many people offered her support during her illness. Her family shed tears. People donated money to a GoFundMe account set up by her sister.
“I’m upset because all these people were so distraught about me when I could have had one stupid, lousy shot. How selfish can I be? How reckless? I feel guilty — one little shot. It literally took two seconds for them to give it to me.”
Pregnant mothers have more to fear, Amy said, from being unvaccinated and getting sick than they do from that simple poke in the arm. For her, a joyous time was forever marred.
“COVID didn’t just happen to me,” Amy said. “It happened to my entire family and everybody who knows me. Not getting vaccinated was probably the worst decision of my life.”
Media contact: Ken Garcia at kdgarcia@ufl.edu or 352-265-9408
About the author
