Prevent and Protect Yourself from HPV
This year, the University of Florida Health Cancer Center is recognizing March 4, International HPV Awareness Day, by equipping you with the information you…

Update your location to show providers, locations, and services closest to you.
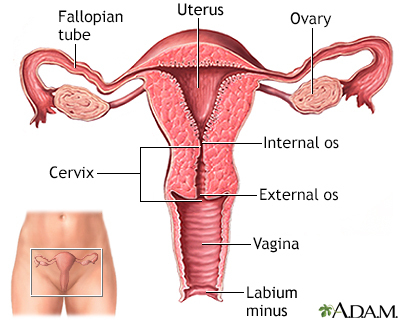
The Pap test mainly checks for changes that may turn into cervical cancer. Cells scraped from the opening of the cervix are examined under a microscope. The cervix is the lower part of the uterus (womb) that opens at the top of the vagina.
This test is sometimes called a Pap "smear" or "cervical cytology."
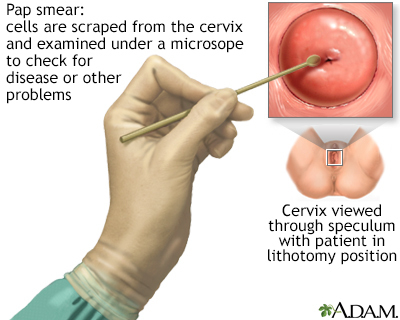
Papanicolaou test; Pap smear; Cervical cancer screening - Pap test; Cervical intraepithelial neoplasia - Pap; CIN - Pap; Precancerous changes of the cervix - Pap; Cervical cancer - Pap; Squamous intraepithelial lesion - Pap; LSIL - Pap; HSIL - Pap; Low-grade Pap; High-grade Pap; Carcinoma in situ - Pap; CIS - Pap; ASCUS - Pap; Atypical glandular cells - Pap; AGUS - Pap; Atypical squamous cells - Pap; HPV - Pap; Human papilloma virus - Pap cervix - Pap; Colposcopy - Pap; Cervical cytology
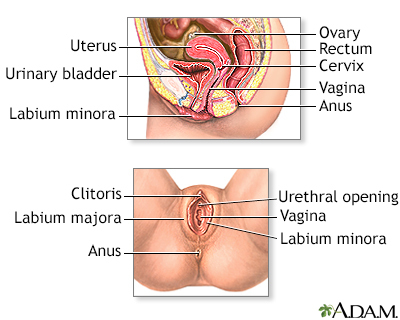
You lie on a table and place your feet in footrests. Your health care provider gently inserts an instrument called a speculum into the vagina to open it slightly. This allows the provider to see the cervix.
Cells are gently collected from the cervix area. The sample of cells is sent to a lab for examination.
Tell your provider if you:
DO NOT do the following for 24 hours before the test:
Try not to schedule your Pap test for when you have your period, but if you are having unexpected bleeding, do not cancel your exam. Your provider will determine if the Pap test can still be done.
For your comfort, you may want to empty your bladder just before the test.
A Pap test causes little to no discomfort for most people. It can cause some discomfort, similar to menstrual cramps. You may also feel some pressure during the exam.
You may bleed a little bit after the test.
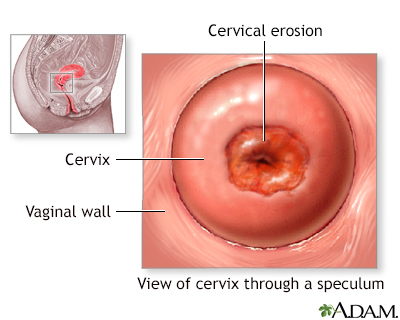
The Pap test looks for changes in cervical cells that may turn into cervical cancer. Most cervical cancers can be avoided if you have screenings according to the recommended schedule.
You should start having Pap tests at age 21 and continue having them every 3 years.
If you are over age 30 you can do any of the following:
You may not need to have a Pap test if you have had a total hysterectomy (uterus and cervix removed) and have not had abnormal tests in the past.
Most people can stop having Pap tests after age 65 if they've had normal tests in the past. Ask your provider when you should stop screening.
A normal result means there are no abnormal cells present. The Pap test is not 100% accurate, and this is why repeat testing is recommended. Because cervical cancer develops very slowly, repeat Pap tests usually find changes in time for treatment before cancer develops.
The most common abnormal Pap test results are:
Atypical squamous cells of undetermined significance (ASC-US)
Low-grade squamous intraepithelial lesion (LSIL)
Atypical squamous cells, cannot rule out HSIL (ASC-H)
High-grade squamous intraepithelial lesion (HSIL)
Atypical glandular cells (AGC)


Fontham ETH, Wolf AMD, Church TR, Etzioni R, Flowers CR, Herzig A, Guerra CE, Oeffinger KC, Shih YT, Walter LC, Kim JJ, Andrews KS, DeSantis CE, Fedewa SA, Manassaram-Baptiste D, Saslow D, Wender RC, Smith RA. Cervical cancer screening for individuals at average risk: 2020 guideline update from the American Cancer Society. CA Cancer J Clin. 2020 Sep;70(5):321-346. Epub 2020 Jul 30. PMID: 32729638 pubmed.ncbi.nlm.nih.gov/32729638/.
Newkirk GR. Pap smear and related techniques for cervical cancer screening. In: Fowler GC, ed. Pfenninger and Fowler's Procedures for Primary Care. 4th ed. Philadelphia, PA: Elsevier; 2020:chap 120.
Perkins RB, Guido RS, Castle PE, Chelmow D, Einstein MH, Garcia F, Huh WK, Kim JJ, Moscicki AB, Nayar R, Saraiya M, Sawaya GF, Wentzensen N, Schiffman M; 2019 ASCCP Risk-Based Management Consensus Guidelines Committee. 2019 ASCCP Risk-Based Management Consensus Guidelines for Abnormal Cervical Cancer Screening Tests and Cancer Precursors. J Low Genit Tract Dis. 2020 Apr;24(2):102-131. Erratum in: J Low Genit Tract Dis. 2020 Oct;24(4):427. PMID: 32243307; PMCID: PMC7147428 pubmed.ncbi.nlm.nih.gov/32243307/.
Salcedo MP, Phoolcharoen N, Schmeler KM. Intraepithelial neoplasia of the lower genital tract (cervix, vagina, vulva): etiology, screening, diagnosis, management. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 29.
US Preventive Services Task Force, Curry SJ, Krist AH, Owens DK, et al. Screening for cervical cancer: US Preventive Services Task Force recommendation statement. JAMA. 2018;320(7):674-686. PMID: 30140884 pubmed.ncbi.nlm.nih.gov/30140884/.






Our community and patient programs provide great value to patients, families and loved ones. People can find support, educational materials, expert consultants and more. In most instances, these programs are offered free of charge.
Provides primary medical care services at no cost to the patient.
This year, the University of Florida Health Cancer Center is recognizing March 4, International HPV Awareness Day, by equipping you with the information you…
