Tongue problems
Definition
Tongue problems include pain, swelling, or a change in how the tongue looks.
Alternative Names
Dark tongue; Burning tongue syndrome - symptoms
Considerations
The tongue is mainly made up of muscles. It is covered with a mucous membrane. Small bumps (papillae) cover the surface of back part of the tongue.
- Between the papillae are the taste buds, which allow you to taste.
- The tongue moves food to help you chew and swallow.
- The tongue also helps you form words.
There are many different reasons for changes in the tongue's function and appearance.
PROBLEMS MOVING THE TONGUE
Tongue movement problems are most often caused by nerve damage. Rarely, problems moving the tongue may also be caused by a disorder where the band of tissue that attaches the tongue to the floor of the mouth is too short. This is called ankyloglossia.
Tongue movement problems may lead to:
- Breastfeeding problems in newborns
- Difficulty moving food during chewing and swallowing
- Speech problems
TASTE PROBLEMS
Taste problems can be caused by:
- Damage to the taste buds
- Nerve problems
- Side effects of some medicines
- An infection, or other condition
The tongue normally senses sweet, salty, sour, and bitter tastes. Other "tastes" are actually a function of the sense of smell.
INCREASED SIZE OF THE TONGUE
Tongue swelling occurs with:
- Acromegaly
- Amyloidosis
- Down syndrome
- Myxedema
- Rhabdomyoma
- Prader Willi Syndrome
- Tongue cancer
The tongue may get wider in people who have no teeth and do not wear dentures.
Sudden swelling of the tongue can happen due to an allergic reaction or a side effect of medicines.
COLOR CHANGES
Color changes may occur when the tongue becomes inflamed (glossitis). Papillae (bumps on the tongue) are lost, causing the tongue to appear smooth. Geographic tongue is a patchy form of glossitis where the location of inflammation and the appearance of the tongue change from day to day.
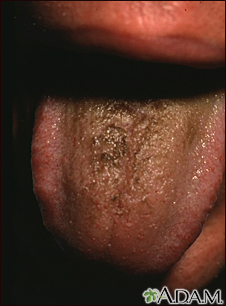
HAIRY TONGUE
Hairy tongue is a condition in which the tongue looks hairy or furry. It can sometimes be treated with antifungal medicine.
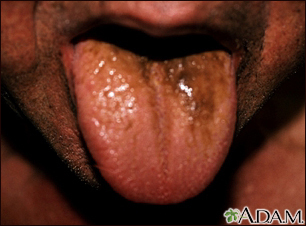
BLACK TONGUE
Sometimes the upper surface of the tongue turns black or brown in color. This is an unsightly condition, but it is not harmful.
PAIN IN THE TONGUE
Pain may occur with glossitis and geographic tongue. Tongue pain may also occur with:
- Diabetic neuropathy
- Leukoplakia
- Mouth ulcers
- Oral cancer
After menopause, some women have a sudden feeling that their tongue has been burned. This is called burning tongue syndrome or idiopathic glossopyrosis. There is no specific treatment for burning tongue syndrome, but capsaicin (the ingredient that makes peppers spicy) can offer relief to some people.
Causes
Minor infections or irritations are the most common cause of tongue soreness. Injury, such as biting the tongue, can cause painful sores. Heavy smoking can irritate the tongue and make it painful.
A benign ulcer on the tongue or elsewhere in the mouth is common. This is called a canker sore and can appear for no known reason.
Possible causes of tongue pain include:
- Anemia
- Cancer
- Dentures that irritate the tongue
- Oral herpes (ulcers)
- Neuralgia
- Pain from teeth and gums
- Pain from the heart
Possible causes of tongue tremor:
- Neurological disorder
- Overactive thyroid
Possible causes of white tongue:
- Local irritation
- Smoking and alcohol use
Possible causes of smooth tongue:
- Anemia
- Vitamin B12 deficiency
Possible causes of red (ranging from pink to reddish-purple) tongue:
- Folic acid and vitamin B12 deficiency
- Pellagra
- Pernicious anemia
- Plummer-Vinson syndrome
- Sprue
Possible causes of tongue swelling:
- Acromegaly
- Allergic reaction to food or medicine
- Amyloidosis
- Angioedema
- Beckwith syndrome
- Cancer of the tongue
- Congenital micrognathia
- Down syndrome
- Hypothyroidism
- Infection
- Leukemia
- Lymphangioma
- Neurofibromatosis
- Pellagra
- Pernicious anemia
- Strep infection
- Tumor of the pituitary gland
Possible causes of a hairy tongue:
- AIDS
- Antibiotic therapy
- Drinking coffee
- Dyes in drugs and food
- Chronic medical conditions
- Overuse of mouthwashes containing oxidizing or astringent ingredients
- Radiation of the head and neck
- Tobacco use
Home Care
Practicing good oral self-care can help hairy tongue and black tongue. Be sure to eat a well-balanced diet.
Canker sores will heal on their own.
See your dentist if you have a tongue problem caused by dentures.
Antihistamines can help relieve a swollen tongue caused by allergies. Avoid the food or drug that causes the tongue swelling. Seek medical attention right away if swelling is starting to make breathing difficult.
When to Contact a Medical Professional
Call your health care provider if your tongue problem persists.
What to Expect at Your Office Visit
The provider will perform a physical exam, to look closely at the tongue. You may be asked questions such as:
- When did you first notice the problem?
- Have you had similar symptoms before?
- Do you have pain, swelling, breathing problems, or difficulty swallowing? Are there problems with speaking or moving the tongue?
- Have you noticed changes in taste?
- Do you have a tongue tremor?
- What makes the problem worse? What have you tried that helps?
- Do you wear dentures?
- Are there problems with the teeth, gums, lips, or throat? Does the tongue bleed?
- Do you have a rash or fever? Do you have allergies?
- What medicines do you take?
- Do you use tobacco products or drink alcohol?
You may need blood tests or a biopsy to check for other conditions.
Treatment depends on the cause of the tongue problem. Possible treatments include:
- If nerve damage has caused a tongue movement problem, the condition must be treated. Therapy may be needed to improve speech and swallowing.
- Ankyloglossia may not need to be treated, unless you have speech or swallowing problems. Surgery to release the tongue can relieve the problem.
- Medicine may be prescribed for mouth ulcers, leukoplakia, oral cancer, and other mouth sores.
- Anti-inflammatory medicines may be prescribed for glossititis and geographic tongue.
Gallery
References
James WD, Elston DM, Treat JR, Rosenbach MA, Neuhaus IM. Pruritus and neurocutaneous dermatoses. In: James WD, Elston DM, Treat JR, Rosenbach MA, Neuhaus IM, eds. Andrews' Diseases of the Skin: Clinical Dermatology. 13th ed. Philadelphia, PA: Elsevier; 2020:chap 4.
Neville BW, Damm DD, Allen CM, Chi AC. Oral manifestations of systemic diseases. In: Neville BW, Damm DD, Allen CM, Chi AC, eds. Oral and Maxillofacial Pathology. 4th ed. St Louis, MO: Elsevier; 2016:chap 17.
Pham KL, Mirowski GW. Oral diseases and oral manifestations of gastrointestinal and liver disease. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 24.
