Definition
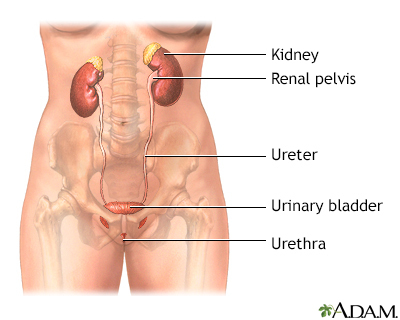
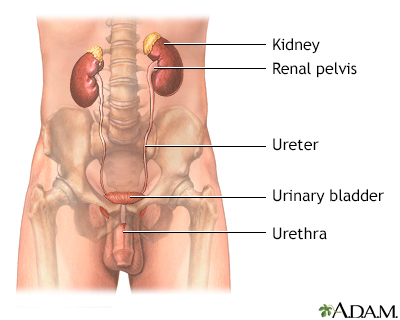
Urethral stricture is an abnormal narrowing of the urethra. The urethra is the tube that carries urine out of the body from the bladder.
Causes
A urethral stricture may be caused by swelling or scar tissue from surgery. It can also occur after an infection or injury. Rarely, it may be caused by pressure from a growing tumor near the urethra.
Other factors that increase the risk for this condition include:
Strictures that are present at birth (congenital) are rare. The condition is also rare in women.
Exams and Tests
A physical exam may show the following:
- Decreased urinary stream
- Discharge from the urethra
- Enlarged bladder
- Enlarged or tender lymph nodes in the groin
- Enlarged or tender prostate
- Hardness on the under surface of the penis
- Redness or swelling of the penis
Sometimes, the exam reveals no abnormalities.
Tests include the following:
Treatment
The urethra may be widened (dilated) during cystoscopy. Topical numbing medicine will be applied to the area before the procedure. A thin instrument is inserted into the urethra to stretch it. You may be able to treat your stricture by learning to dilate the urethra at home.
If urethral dilation cannot correct the condition, you may need surgery. The type of surgery will depend on the location and length of the stricture. If the narrowed area is short and not near the muscles that control the exit from the bladder, the stricture may be cut or dilated.
A surgery called an open urethroplasty may be done for longer strictures. This surgery involves removing the diseased area. The urethra is then rebuilt. The results vary, depending on the size and location of the stricture, the number of treatments you have had, and the surgeon's experience.
In acute cases when you cannot pass urine, a suprapubic catheter may be placed. This is an emergency treatment. This allows the bladder to drain through the abdomen.
There are currently no drug treatments for this disease. If no other treatments work, a urinary diversion called an appendicovesicostomy (Mitrofanoff procedure) or another type of surgery may be done. This lets you drain your bladder through the wall of the abdomen using a catheter or a stoma bag.
Outlook (Prognosis)
The outcome is often excellent with treatment. Sometimes, treatment needs to be repeated to remove scar tissue.
A urethral stricture may totally block urine flow. This can cause sudden urinary retention. This condition must be treated quickly. Long-term blockage can lead to permanent bladder or kidney damage.
When to Contact a Medical Professional
Contact your health care provider if you have symptoms of urethral stricture.
Prevention
Practicing safer sex may decrease the risk of getting STIs that may cause a urethral stricture.
Treating urethral stricture quickly may prevent kidney or bladder complications.
References
Babu TM, Urban MA, Augenbraun MH. Urethritis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 107.
Elder JS. Obstruction of the urinary tract. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 555.
Virasoro R, Jordan GH, McCammon KA. Surgery for benign disorders of the penis and urethra. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 82.