Slit-lamp exam
Definition
The slit-lamp examination looks at structures that are at the front of the eye.
Alternative Names
Biomicroscopy
How the Test is Performed
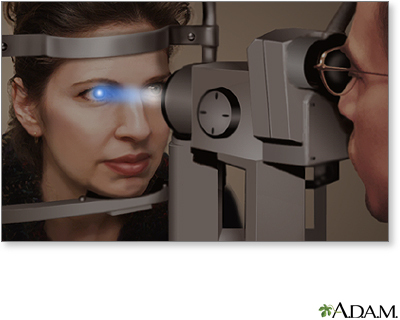
The slit-lamp is a low-power microscope combined with a high-intensity light source that can be focused as a thin beam.
You will sit in a chair with the instrument placed in front of you. You will be asked to rest your chin and forehead on a support to keep your head steady.
The health care provider will examine your eyes, especially the eyelids, cornea, conjunctiva, sclera, and iris. Often a yellow dye (fluorescein) is used to help examine the cornea and tear layer. The dye is either added as an eyedrop. Or, the provider may touch a fine strip of paper stained with the dye to the white of your eye. The dye rinses out of the eye with tears as you blink.
Next, drops may be placed in your eyes to widen (dilate) your pupils. The drops take about 15 to 20 minutes to work. The slit-lamp examination is then repeated using another small lens held close to the eye, so the back of the eye can be examined.
How to Prepare for the Test
No special preparation is needed for this test.
How the Test will Feel
Your eyes will be sensitive to light for a few hours after the exam if dilating drops are used.
Why the Test is Performed
This test is used to examine the:
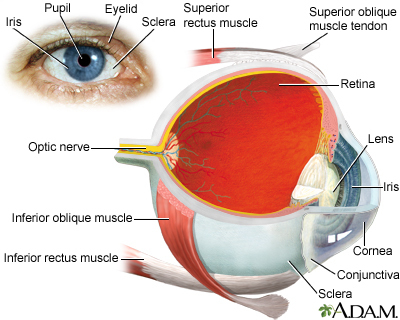
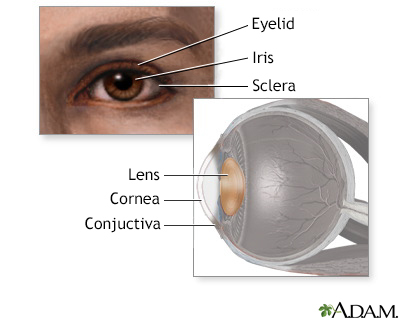
- Conjunctiva (the thin membrane that covers the inner surface of the eyelid and the white part of the eyeball)
- Cornea (the clear outer lens on the front of the eye)
- Eyelids
- Iris (colored part of the eye between the cornea and lens)
- Lens
- Sclera (the white outer coating of the eye)
Normal Results
Structures in the eye are found to be normal.
What Abnormal Results Mean
The slit lamp exam may detect many diseases of the eye, including:
- Clouding of the lens of the eye (cataract)
- Injury to the cornea
- Dry eye syndrome
- Loss of sharp vision due to macular degeneration
- Separation of the retina from its supporting layers (retinal detachment)
- Blockage in a small artery or vein that carries blood to or from the retina (retinal vessel occlusion)
- Inherited degeneration of the retina (retinitis pigmentosa)
- Swelling and irritation of the uvea (uveitis), the middle layer of the eye
This list does not include all possible diseases of the eye.
Risks
If you receive drops to dilate your eyes for the ophthalmoscopy, your vision will be blurred.
- Wear sunglasses to protect your eyes from sunlight, which can damage your eyes.
- Have someone drive you home.
- The drops usually wear off in several hours.
In rare cases, the dilating eyedrops cause:
- An attack of narrow-angle glaucoma
- Dizziness
- Dryness of the mouth
- Flushing
- Nausea and vomiting
Gallery
References
Atebara NH, Miller D, Thall EH. Ophthalmic instruments. In: Yanoff M, Duker JS, eds. Ophthalmology. 5th ed. Philadelphia, PA: Elsevier; 2019:chap 2.5.
Chuck RS, Dunn SP, Flaxel CJ; American Academy of Ophthalmology Preferred Practice Pattern Committee, et al. Comprehensive adult medical eye evaluation preferred practice pattern. Ophthalmology. 2021;128(1):1-29. doi.org/10.1016/j.ophtha.2020.10.024. Published November 12, 2020.
Prokopich CL, Hrynchak P, Flanagan JG, Hynes AF, Chisholm C. Ocular health assessment. In: Elliott DB, ed. Clinical Procedures in Primary Eye Care. 5th ed. Philadelphia, PA: Elsevier; 2021:chap 7.