Erysipelas
Definition
Erysipelas is a type of skin infection. It affects the outermost layer of the skin and the local lymph nodes.
Alternative Names
Strep infection - erysipelas; Streptococcal infection - erysipelas; Cellulitis - erysipelas
Causes
Erysipelas is usually caused by group A streptococcus bacteria. The condition may affect both children and adults.
Some conditions that can lead to erysipelas are:
- A cut in the skin
- Problems with drainage through the veins or lymph system
- Skin sores (ulcers)
Symptoms
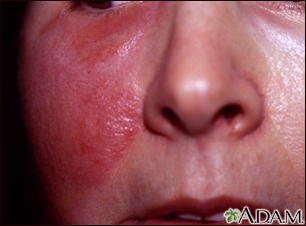
The infection occurs on the legs or arms most of the time. It may also occur on the face and trunk.
Symptoms of erysipelas may include:
- Fever and chills
- Skin sore with a sharp raised border. As the infection spreads, the skin is painful, very red, swollen, and warm. Blisters on the skin can form.
Exams and Tests
Erysipelas is diagnosed based on how the skin looks. A biopsy of the skin is usually not needed.
Treatment
Antibiotics are used to get rid of the infection. If the infection is severe, antibiotics may need to be given through an intravenous (IV) line.
People who have repeated episodes of erysipelas may need long-term antibiotics.
Outlook (Prognosis)
With treatment, the outcome is good. It may take a few weeks for the skin to return to normal. Peeling is common as the skin heals.
Possible Complications
Sometimes the bacteria that cause erysipelas may travel to the blood. This results in a condition called bacteremia. When this happens, the infection may spread to the heart valves, joints, and bones.
Other complications include:
- Return of infection
- Septic shock (a dangerous body-wide infection)
When to Contact a Medical Professional
Contact your health care provider if you have a skin sore or other symptoms of erysipelas.
Prevention
Keep your skin healthy by avoiding dry skin and preventing cuts and scrapes. This may reduce the risk for erysipelas.
Gallery

References
Bryant AE, Stevens DL. Streptococcus pyogenes. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 197.
Patterson JW. Bacterial and rickettsial infections. In: Patterson JW, ed. Weedon's Skin Pathology. 5th ed. Philadelphia, PA: Elsevier Limited; 2021:chap 24.