What to Know Before Getting a Vasectomy
Getting a vasectomy, sometimes called male sterilization, is a decision that more men are choosing to make, with an 850% increase for the search term "where…

Update your location to show providers, locations, and services closest to you.
Our fertility specialists offer multifaceted and multispecialty services to make sure that every aspect of male infertility and its potential associated conditions can be analyzed. The UF Health Reproductive Medicine team collaborates with urologists to ensure fast-track evaluation and management of the male partner, which further enhances our treatment success rates.
Read an inspiring story on how our team helped a patient successfully overcome infertility struggles.
Evaluation of a man’s fertility can be a multistep process for clinicians and patients alike. There are a wide range of potential causes that may contribute to reproductive difficulties, including genetic, congenital, medical, surgical, environmental and psychosocial etiologies.
These causes can include genitourinary anomalies at birth, previous reconstructive surgeries, exposures to chemotherapy or radiation, certain hormone therapies, smoking, endocrine disorders such as diabetes mellitus, previous sexually transmitted diseases, neurologic disorders, or trauma.
Infertility affects approximately 15% of couples that attempt to conceive. Male factor infertility may be attributable to approximately 50% of infertile relationships: 30% of couples due to a significant male factor alone and 20% with combined male and female factors. Infertility may be considered to exist after 12 months of attempted conception without any form of contraception. This should be considered in the setting that pregnancy rates through intercourse in couples are approximately 20-25% per month and 90% at one year.
The fertility workup requires an assessment of each relationship partner involved. A general workup includes a thorough review of the patient’s history and a physical. A discussion of the duration of a couple’s infertility, previous attempted treatments and prior pregnancies is crucial. The history also includes a reproductive and sexual history and identifying any past medical and surgical history, as these will help to identify common causes of infertility.
The physical exam will also give important information regarding the overall health of the male, and a focused genital exam may reveal varicoceles (dilated varicose veins), spermatic cord abnormalities or testicular concerns. Other conditions that could potentially lead to fertility issues include premature ejaculation, erectile dysfunction and Peyronie disease.
In addition to patient history and a physical, bloodwork is routinely performed to evaluate the hormonal interaction between the hypothalamus, pituitary and testicles.
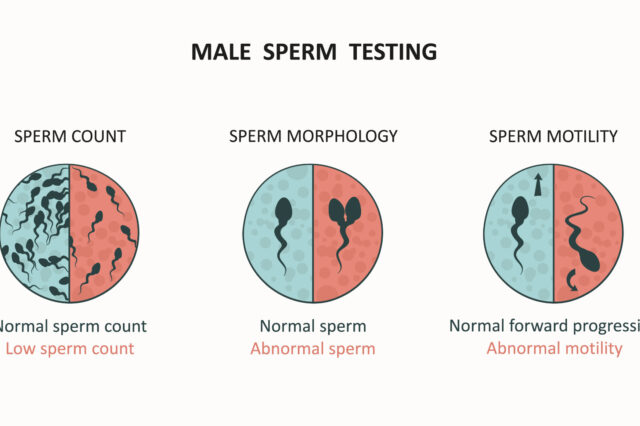
Importantly, a semen analysis should be performed. The semen analysis is arguably the most important laboratory evaluation of the male undergoing an infertility workup. At minimum, two semen analyses should be obtained with a similar duration of abstinence for consistency. The ideal abstinence period is at least 2-3 days. Shorter periods may give artificially low semen concentrations, whereas longer periods may affect sperm motility.
After the initial workup is performed, testing such as imaging, additional semen investigation or genetic evaluation may also be warranted.
The treatment options for male infertility depend on the cause. If a hormonal imbalance or production problem is causing the lack or decreased sperm production, medication or adjustments to the hormonal axis may be able to restore or increase sperm production. This may include testosterone levels for example.
If the cause is an obstruction (as in the case of a previous vasectomy, scarring or inflammation from infection, or epididymal cysts), surgical treatment to restore patency of the vas deferens or to bypass the obstruction are options. Additionally, sperm retrieval from the testicle may be performed directly for many of these cases.
There are a number of procedures our male infertility physicians can offer to help couples achieve their dream of starting a family. They include:

Getting a vasectomy, sometimes called male sterilization, is a decision that more men are choosing to make, with an 850% increase for the search term "where…

A few years ago, Nicholas and his wife moved back to Nicholas home state of Florida to complete his training at UF Health. Their plan was that as soon as their…