UF Health surgeon performs first-of-its-kind computer-assisted surgery in U.S. using new technology
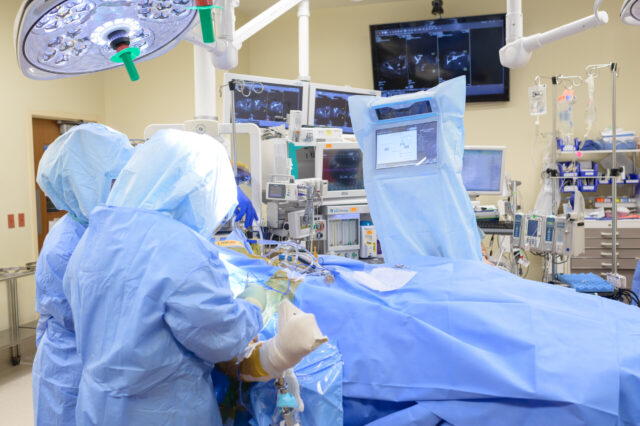
A University of Florida Health orthopaedic surgeon is one of two nationally to perform the first computer-assisted shoulder replacement surgery in the U.S. using a new technology allowing live navigation of the operative site.
The technology, ExactechGPS Total Shoulder Application, provides the surgeon with a real-time 3-D computer model of a patient’s shoulder during surgery. It does this by combining CT scan images with data from instruments mounted with tiny infrared cameras.
The combination gives the surgeon a road map for the placement of implant screws with tolerances of 2 millimeters, besting what is possible with the human eye. The technology is expected to produce more secure, durable implants with fewer complications.
The surgery was performed May 31 by Thomas Wright, M.D., a UF professor and surgeon with the UF Health Orthopaedics and Sports Medicine Institute and director of the Interdisciplinary Center for Musculoskeletal Training and Research. He was assisted by Larry D. Waldrop, M.D.
Wright’s surgery was done simultaneously with an identical procedure performed on a second patient by Richard Jones, M.D., of Pardee UNC Healthcare’s Southeastern Sports Medicine & Orthopedics in Hendersonville, N.C., near Ashville. Since both Wright and Jones worked on the design of the technology with Exactech, a Gainesville medical device manufacturer, they decided to share the honor of being the first in the U.S. to use the technology.
“This dramatically improves accuracy,” said Wright. “It certainly allows you to place things exactly where you want to place them. I think we’re probably good with the human eye to 3 to 5 millimeters. And that’s surgeons who do a lot of them. But even that is not nearly as good as this technology. This thing would kill me every time. It’d be like playing against a chess champion.”
Wright has performed an estimated 2,500 shoulder replacement surgeries, considered a high volume for the procedure. About 100,000 Americans have shoulder replacement surgeries each year, according to Exactech. That compares with about 900,000 hip and knee replacements.
Wright said ExactechGPS will allow surgeons who typically perform fewer of these operations to place bone screws far closer to the mark.
“The biggest thing for this really will be people who don’t do this operation very often who have standard deviations that are really big,” Wright said. “It’s kind of a hard operation. The outcome for low-volume surgeons is not predictable, whereas ours are much tighter because we do four to 10 a week. But this will help the low-volume surgeons because then they can obtain standard deviations just like the rest of us or better.”
ExactechGPS Shoulder Application has been used in Europe and Australia for the past eight months. But the company recently received permission from the Food and Drug Administration to use the technology in the United States.
Exactech’s software allows surgeons to virtually plan the operation using a 3-D anatomical model of the patient’s shoulder with images from a CT scan. Wright noted it can be difficult to get a complete view of a patient’s shoulder anatomy during the actual surgery.
But the software allows the surgeon to guide a bone drill mounted with an infrared camera to the exact location plotted out during pre-op planning and determine drilling depth, screw placement and the ability to adjust the pre-op surgical plan, if necessary. The cameras communicate with a computer tablet that displays a digital model of the patient’s shoulder, showing a drill location like a dot on a smartphone’s map app.
Wright’s surgery was performed on the right shoulder of Mercia Reid, 74, a Gainesville woman whose severe arthritis caused extreme pain in her joints. Wright had already performed a successful shoulder replacement on her left arm without the new technology.
Reid said she hoped the new technology would help many others in her situation, allowing for safer, more successful surgeries.
“So far, it’s been good,” she said of her recovery a week after the surgery. “I have to keep reminding myself to keep my arm down and not use my hand. It’s been feeling good.”
Wright said he hopes the technology might be adapted to other types of orthopaedic surgeries. “This is great,” he said. “But this is first grade. We will eventually be able to apply it to more osseous structures once you’ve got a really adaptable software platform.”
About the author
