Tests show common diabetes drug slows age-related vision loss
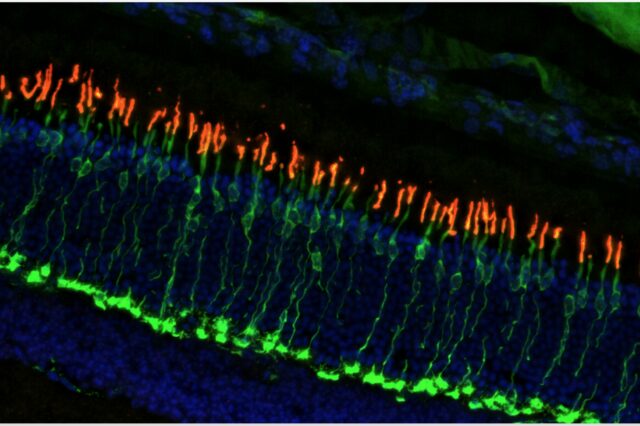
 A common and affordable Type 2 diabetes drug may someday have a new use in fighting vision loss, say University of Florida Health researchers who tested it in mouse models and found it slowed the loss of photoreceptors in the eye that lead to blindness.
A common and affordable Type 2 diabetes drug may someday have a new use in fighting vision loss, say University of Florida Health researchers who tested it in mouse models and found it slowed the loss of photoreceptors in the eye that lead to blindness.
Metformin is given to patients with diabetes to reduce the amount of sugar in the blood by instructing muscles and other cells to use glucose for energy. Now, researchers know the drug also stimulates metabolism in the eye’s retinal cells. That added energy production ultimately makes these cells less susceptible to age-related macular degeneration, a common eye disorder.
“It allows these cells in the retina to be hardier and more resistant to damage,” said John D. Ash, Ph.D., an ophthalmology researcher in the UF College of Medicine.
The findings were published Sept. 24 in the Proceedings of the National Academy of Sciences.
Age-related macular degeneration, or AMD, causes a progressive loss of central vision. It affects more than 10 million people in the United States and is the leading cause of vision loss in older adults, according to the Foundation Fighting Blindness. Currently, there is no cure for AMD. The current treatment — a mix of vitamins and antioxidants — has moderate beneficial effects in certain patients, a 2011 study by other researchers found.
The new findings are particularly encouraging because metformin is an economical, widely used medication with few significant side effects, Ash said. Because it is an existing medication, testing its vision-protecting effects in humans could happen sooner than if it were a new drug, he added.
Ash said he focused on metformin because it can prompt cells to gather and use glucose, a simple sugar, as an energy source. Photoreceptors and their supporting cells in the retina are energy hungry, so keeping them fully powered up can reduce DNA damage and reduce the damaging effects of oxygen being metabolized. Metformin produces its beneficial eye effects by activating a protective enzyme known as adenosine monophosphate-activated protein kinase, or AMPK, the researchers found.
To establish their findings, the researchers tested metformin in three different mouse models of retinal degeneration. The drug was able to protect photoreceptors from light damage and delay degeneration of the light-sensitive rod and cone cells in the retina. It also made the supporting cells that nourish retinal visual cells more resistant to damage, they found. After eight weeks, metformin-treated mice retained more than 50 percent of cone cell activity, whereas untreated mice did not respond to light flashes used as visual cues.
The drug also performed well in tests that mimicked the cell-damaging effect that occurs when oxygen is metabolized. That process, known as oxidative stress, creates a risk of early macular degeneration. Mice treated with metformin retained 50 to 90 percent of their retinal-support cells, the researchers found. Overall, the drug delivered a 30 percent increase in the lifespan of photoreceptors.
Ash said metformin is not likely a magic bullet for AMD, partly because the disease’s effects in human aren’t fully reproducible in mice. Still, his research suggests that the drug has the potential to reduce vision loss in patients with AMD. Metformin could prevent patients from progressing from early to advanced stages of macular degeneration, he theorized.
“For someone who’s 80 years old and going blind, maybe this drug gives them another 10 years of vision,” he said.
 Researchers hope metformin’s status as a common, established medication can expedite testing in humans as a potential sight-saving treatment.
Researchers hope metformin’s status as a common, established medication can expedite testing in humans as a potential sight-saving treatment.
“It’s a safe drug that people take on a daily basis. It deserves a clinical trial to see if we can delay age-related macular degeneration in people,” Ash said.
Funding for the study was provided by Research to Prevent Blindness, the Foundation Fighting Blindness and the National Eye Institute.
About the researcher: John D. Ash, Ph.D., is an associate professor and the Francis M. Bullard Eminent Scholar Chair in Ophthalmic Sciences in the UF College of Medicine’s department of ophthalmology research.
About the author
