Patent urachus repair
Definition
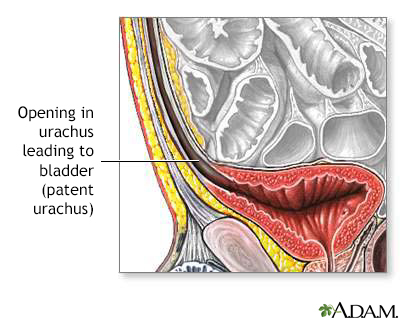
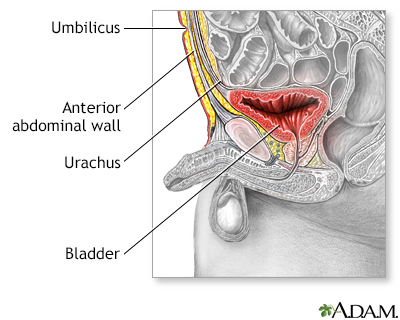
Patent urachus repair is surgery to fix a bladder defect. In an open (or patent) urachus, there is an opening between the bladder and the belly button (navel). The urachus is a tube between the bladder and the belly button that is present before birth. In most cases, it closes along its full length before the baby is born. An open urachus occurs mostly in infants.
Alternative Names
Patent urachal tube repair
Description
Children who have this surgery will have general anesthesia (asleep and pain-free).
The surgeon will make a cut in the child's lower belly. Next, the surgeon will find the urachal tube and remove it. The bladder opening will be repaired, and the cut will be closed.
The surgery can also be done with a laparoscope. This is an instrument that has a tiny camera and light on the end.
- The surgeon will make 3 small surgical cuts in the child's belly. The surgeon will insert the laparoscope through one of these cuts and other tools through the other cuts.
- The surgeon uses the tools to remove the urachal tube and close off the bladder and area where the tube connects to the umbilicus (belly button).
This surgery can be done in children as young as 6 months.
Why the Procedure Is Performed
Surgery is recommended for a patent urachus that does not close after birth. Problems that can occur when a patent urachal tube is not repaired include:
- A higher risk for urinary tract infections
- A higher risk for cancer of the urachal tube later in life
- Continued leakage of urine from the urachus
Risks
Risks for any anesthesia are:
- Reactions to medicines
- Breathing problems
Risks for any surgery are:
- Bleeding
- Infection
- Blood clots in the legs that may travel to the lungs
Additional risks for this surgery are:
- Bladder infection.
- Bladder fistula (connection between the bladder and the skin) -- if this happens, a catheter (thin tube) is inserted into the bladder to drain urine. It is left in place until the bladder heals or additional surgery may be needed.
Before the Procedure
The surgeon may ask your child to have:
- A complete medical history and physical exam.
- Kidney ultrasound.
- Sinogram of the urachus. In this procedure, a radio-opaque dye called contrast is injected into the urachal opening and x-rays are taken.
- Ultrasound of the urachus.
- VCUG (voiding cystourethrogram), a special x-ray to make sure the bladder is working.
- CT scan or MRI.
Always tell your child's health care provider:
- What drugs your child is taking. Include drugs, herbs, vitamins, or any other supplements you bought without a prescription.
- About any allergies your child may have to medicine, latex, tape, or skin cleaner.
During the days before the surgery:
- About 10 days before the surgery, you may be asked to stop giving your child aspirin, ibuprofen (Advil, Motrin), naproxen (Aleve, Naprosyn), warfarin (Coumadin), and any other drugs that make it hard for blood to clot.
- Ask which drugs your child should still take on the day of the surgery.
On the day of the surgery:
- Your child will probably not be able to drink or eat anything for 4 to 8 hours before surgery.
- Give your child any drugs you have been told your child should have with a small sip of water.
- Your child's provider will tell you when to arrive at the hospital.
- The provider will make sure your child has no signs of illness before surgery. If your child is ill, the surgery may be delayed.
After the Procedure
Most children stay in the hospital for just a few days after this surgery. Most recover rapidly. Children can eat their normal foods once they start eating again.
Before leaving the hospital, you will learn how to care for the wound or wounds. If Steri-Strips were used to close the wound, they should be left in place until they fall off on their own in about a week.
You may get a prescription for antibiotics to prevent infection and for a safe medicine to use for pain.
Outlook (Prognosis)
The outcome is most often excellent.
Gallery
References
Katz A, Richardson W. Surgery. In: Zitelli BJ, McIntire SC, Nowalk AJ, eds. Zitelli and Davis' Atlas of Pediatric Physical Diagnosis. 7th ed. Philadelphia, PA: Elsevier; 2018:chap 18.
Martin AD, Roth CC. Bladder anomalies in children. In: Partin AW, Domochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 30.
Patel RM, Kaler KS, Landman J. Fundamentals of laparoscopic and robotic urologic surgery. In: Partin AW, Domochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 14.
Schoenwolf GC, Bleyl SB, Brauer PR, Francis-West PH. Development of the urinary system. In: Schoenwolf GC, Bleyl SB, Brauer PR, Francis-West PH, eds. Larsen's Human Embryology. 6th ed. Philadelphia, PA: Elsevier; 2021:chap 15.