University of Florida Health is a Leader in Cardiovascular Care
The University of Florida Health Divisions of Cardiovascular Medicine and Surgery are working together as leaders in the care of our patients in Florida and…

Update your location to show providers, locations, and services closest to you.
Treatment options for thoracic aortic aneurysms vary and include medical (monitoring the aneurysm while controlling blood pressure), open and catheter-based endovascular repair.
Your health care provider has recommended an endovascular repair. This is a minimally invasive procedure and when performed to repair a thoracic aortic aneurysm, it is known as a TEVAR, or Thoracic Endovascular Aortic Repair. For this procedure, small incisions are made in your groin. Long, thin tubes known as catheters are guided through using an X-ray to obtain real-time images and a stent graft is inserted where the aneurysm is located (Figure 2).
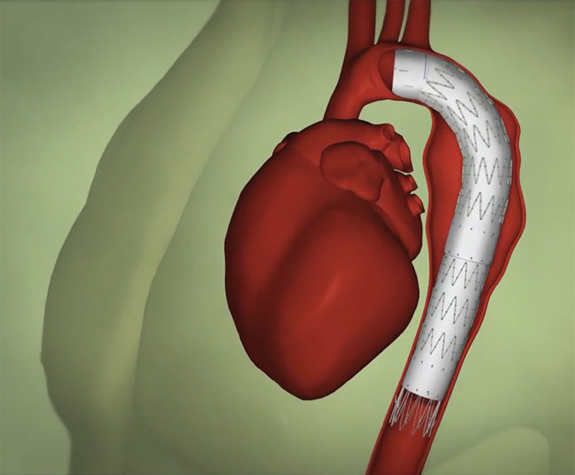
Figure 2. Long, thin tubes known as catheters are guided through using an X-ray to obtain real-time images and a stent graft is inserted where the aneurysm is located.
The stent graft is positioned such that it realigns the weakened blood vessel and prevents the aneurysm from rupturing. Over time, your aorta will shrink back to its normal size.
Here are some tips and information that will help your procedure be as successful as possible:
General anesthesia is used so you will be asleep during the procedure. To prevent spinal cord ischemia (paralysis) by decreasing spinal cord pressure, a spinal drain may be placed in your back if indicated.
Incisions will be created in both your right and left groin. Using wires and catheters, the aorta will be accessed through these small incisions. X-rays will be taken using a special contrast dye that helps visualize blood vessels (Figure 3). Under this direct visualization, a stent graft is guided over the wires into the aorta. Then it is positioned and deployed to cover and exclude the aortic aneurysm.
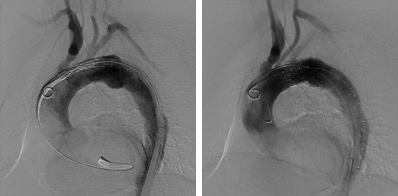
Figure 3. Using wires and catheters, the aorta will be accessed through these small incisions. X-rays will be taken using a special contrast dye that helps visualize blood vessels.
You will be taken to the intensive care unit, or ICU. Once you are medically ready, typically after one or two days, you will move to a medical-surgical unit. You are asked to lay flat in bed until the spinal drain has been discontinued, usually 24 hours after your procedure. When you are tolerating a diet and able to walk, you may leave the hospital two to five days after the endovascular repair.
There are risks associated with every procedure. Those specific to this operation include, but are not limited to:
For two weeks after the endovascular repair, you should not lift anything that weighs more than five to 10 pounds. If you are taking narcotic medications, do not drive or operate heavy machinery as these medications can impair judgment. You may shower and let soap and water run over your incisions, but must pat them dry afterwards. You may return to work when you are cleared by your doctor.
Check your incision daily for signs of infection (redness, increased tenderness, warmth or swelling). If you develop sudden shortness of breath or chest pain, or if you notice changes in color, sensation or strength in your legs, please seek medical
attention immediately.
Over time, stent grafts may have problems such as kinking, migration or leakage and you may or may not experience symptoms. Therefore, you will need lifelong routine surveillance with CT scans. Most problems seen after repair can be managed with endovascular techniques.
At the time of discharge, you will be provided an appointment at one month and six months from the date of repair with a repeat CT scan to evaluate the stent graft and remodeling of the aorta around the graft. After that, follow-up is typically done yearly. It is crucial that you are compliant with the follow-up plan provided to you to ensure the most successful outcome after your procedure.
The University of Florida Health Divisions of Cardiovascular Medicine and Surgery are working together as leaders in the care of our patients in Florida and…
