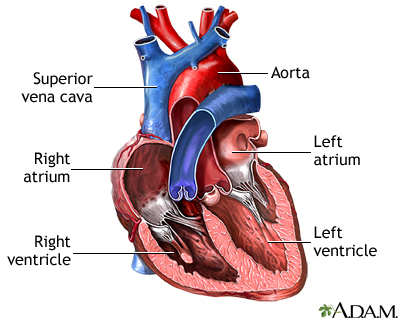
Definition
Palpitations are feelings or sensations that your heart is pounding or racing. They can be felt in your chest, throat, or neck.
You may:
- Have an unpleasant awareness of your own heartbeat
- Feel like your heart skipped or stopped beats
The heart's rhythm may be normal or abnormal when you have palpitations.
Alternative Names
Heartbeat sensations; Irregular heartbeat; Palpitations; Heart pounding or racing
Considerations
Normally the heart beats 60 to 100 times per minute. The rate may drop below 60 beats per minute in people who exercise routinely or take medicines that slow the heart.
If your heart rate is fast (over 100 beats per minute), this is called tachycardia. A heart rate slower than 60 is called bradycardia. An occasional extra heartbeat out of rhythm is known as extrasystole.
Palpitations are not serious most of the time. Sensations representing an abnormal heart rhythm (arrhythmia) may be more serious.
The following conditions make you more likely to have an abnormal heart rhythm:
- Known heart disease at the time the palpitations begin
- Significant risk factors for heart disease
- An abnormal heart valve
- An electrolyte abnormality in your blood -- for example, a low potassium level
Causes
Heart palpitations can be due to:
- Anxiety, stress, panic attack, or fear
- Caffeine intake
- Cocaine, methamphetamine or other stimulant drugs
- Decongestant medications, such as phenylephrine or pseudoephedrine
- Diet pills
- Exercise
- Fever
- Nicotine intake
However, some palpitations are due to an abnormal heart rhythm, which may be caused by:
- Heart disease
- Abnormal heart valve, such as mitral valve prolapse
- Abnormal blood level of potassium
- Certain medicines, including those used to treat asthma, high blood pressure, or heart problems
- Overactive thyroid
- Low level of oxygen in your blood
Home Care
Things you can do to limit palpitations include:
- Lower your intake of caffeine and nicotine. This will often reduce heart palpitations.
- Learn to reduce stress and anxiety. This can help prevent palpitations and help you better manage them when they occur.
- Try deep relaxation or breathing exercises.
- Practice yoga, meditation, or tai chi.
- Get regular exercise.
- Do not smoke.
Once a serious cause has been ruled out by your provider, try not to pay close attention to heart palpitations. This may cause stress. However, contact your provider if you notice a sudden increase or a change in them.
When to Contact a Medical Professional
If you have never had heart palpitations before, see your provider.
Call 911 or the local emergency number if you have:
Call your provider right away if:
- You often feel extra heartbeats (more than 6 per minute or coming in groups of 3 or more).
- You have heart disease or risk factors for heart disease, such as high cholesterol, diabetes, or high blood pressure.
- You have new or different heart palpitations.
- Your pulse is more than 100 beats per minute (without exercise, anxiety, or fever).
- You have related symptoms, such as chest pain, shortness of breath, feeling faint, or loss of consciousness.
What to Expect at Your Office Visit
Your provider will examine you and ask questions about your medical history and symptoms.
You may be asked:
- Do you feel skipped or stopped beats?
- Does your heart rate feel slow or fast when you have the palpitations?
- Do you feel a racing, pounding, or fluttering?
- Is there a regular or irregular pattern to the unusual heartbeat sensations?
- Did the palpitations begin or end suddenly?
- When do the palpitations occur? In response to reminders of a traumatic event? When you are lying down and resting? When you change your body position? When you feel emotional?
- Do you have any other symptoms?
An electrocardiogram may be done.
If you go to an emergency room, you will be connected to a heart monitor. However, most people with palpitations do not need to go to an emergency room for diagnosis and treatment.
If your provider finds you have an abnormal heart rhythm, other tests may be done. This may include:
References
Fang JC, O'Gara PT. History and physical examination: an evidence-based approach. In: Zipes DP, Libby P, Bonow RO, Mann DL, Tomaselli GF, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 11th ed. Philadelphia, PA: Elsevier; 2019:chap 10.
Miller JM, Tomaselli GF, Zipes DP. Diagnosis of cardiac arrhythmias. In: Zipes DP, Libby P, Bonow RO, Mann DL, Tomaselli, GF, Braunwald E, eds. Braunwald's Heart Disease: A Textbook of Cardiovascular Medicine. 11th ed. Philadelphia, PA: Elsevier; 2019:chap 35.
Olgin JE. Approach to the patient with suspected arrhythmia. In: Goldman L, Schafer AI, eds. Goldman-Cecil Medicine. 26th ed. Philadelphia, PA: Elsevier; 2020:chap 56.