The Importance of Colorectal Cancer Screening: How Early Detection Saves Lives
Colorectal cancer ranks as the second leading cause of cancer-related deaths in the United States. Referred to as a “silent killer” due to its lack of…

Update your location to show providers, locations, and services closest to you.
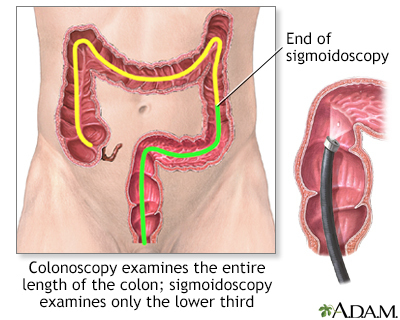
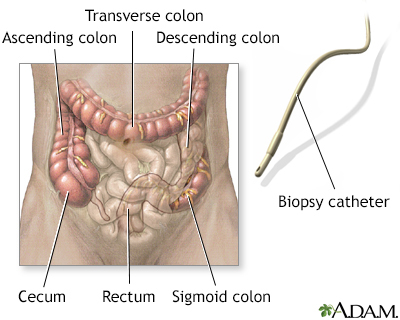
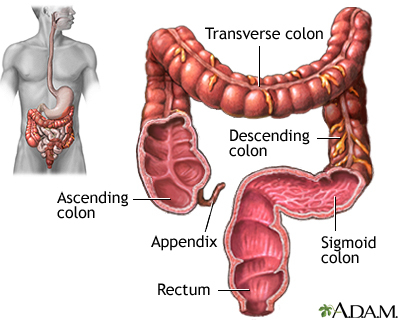
A colonoscopy is an exam that views the inside of the colon (large intestine) and rectum, using a tool called a colonoscope.
The colonoscope has a small camera attached to a flexible tube that can reach the length of the colon.
Colon cancer - colonoscopy; Colorectal cancer - colonoscopy; Colonoscopy - screening; Colon polyps - colonoscopy; Ulcerative colitis - colonoscopy; Crohn disease - colonoscopy; Diverticulitis - colonoscopy; Diarrhea - colonoscopy; Anemia - colonoscopy; Blood in stool - colonoscopy
Colonoscopy is done most often in a procedure room at your doctor's office. It can also be done in the outpatient department of a hospital or medical center.
Your bowel needs to be completely empty and clean for the exam. A problem in your large intestine that needs to be treated may be missed if your intestines are not cleaned out.
Your health care provider will give you the steps for cleansing your bowel. This is called bowel preparation. Steps may include:
You need to drink plenty of clear liquids for 1 to 3 days before the test. Examples of clear liquids are:
You will likely be told to stop taking aspirin, ibuprofen, naproxen, or other blood-thinning medicines for several days before the test. Keep taking your other medicines unless your doctor tells you otherwise.
You will need to stop taking iron pills or liquids a few days before the test, unless your provider tells you it is OK to continue. Iron can make your stool dark black. This makes it harder for the doctor to view inside your bowel.
The medicines will make you sleepy so that you may not feel any discomfort or have any memory of the test.
You may feel pressure as the scope moves inside. You may feel brief cramping and gas pains as air is inserted or the scope advances. Passing gas is necessary and should be expected.
After the exam, you may have mild abdominal cramping and pass a lot of gas. You may also feel bloated and sick to your stomach. These feelings will soon go away.
You should be able to go home about one hour after the test. You must plan to have someone take you home after the test because you will be woozy and unable to drive. The providers will not let you leave until someone arrives to help you.
When you are home, follow instructions on recovering from the procedure. These may include:
Colonoscopy may be done for the following reasons:
Normal findings are healthy intestinal tissues.
Abnormal test results may mean any of the following:
Risks of colonoscopy may include any of the following:
Garber JJ, Chung DC, eds. Colonic polyps and polyposis syndromes. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease: Pathophysiology/Diagnosis/Management. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 126.
Lawler M, Johnson B, Van Schaeybroeck S, et al. Colorectal cancer. In: Niederhuber JE, Armitage JO, Kastan MB, Doroshow JH, Tepper JE, eds. Abeloff's Clinical Oncology. 6th ed. Philadelphia, PA: Elsevier; 2020:chap 74.
National Cancer Institute. Colorectal Cancer Prevention (PDQ) - Health Professional Version. www.cancer.gov/types/colorectal/hp/colorectal-prevention-pdq. Updated April 21, 2022. Accessed May 27, 2022.
Rex DK, Boland CR, Dominitz JA, et al. Colorectal cancer screening: recommendations for physicians and patients from the U.S. Multi-Society Task Force on Colorectal Cancer. Am J Gastroenterol. 2017;112(7):1016-1030. PMID: 28555630 pubmed.ncbi.nlm.nih.gov/28555630/.
US Preventive Services Task Force website. Final recommendation statement. Colorectal cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/colorectal-cancer-screening. Published May 18, 2021. Accessed May 27, 2022.
Wolf AMD, Fontham ETH, Church TR, et al. Colorectal cancer screening for average-risk adults: 2018 guideline update from the American Cancer Society. CA Cancer J Clin. 2018;68(4):250-281. PMID: 29846947 pubmed.ncbi.nlm.nih.gov/29846947/.
Colorectal cancer ranks as the second leading cause of cancer-related deaths in the United States. Referred to as a “silent killer” due to its lack of…

Colorectal cancer is occurring far more often in those under 50 — a trend that’s held for the last decade. With regular screenings, however, the cancer is both…
How far under does a patient need to be during a colonoscopy? As health care costs continue to skyrocket, it’s a question more and more doctors are asking. New research suggests that a growing...